-
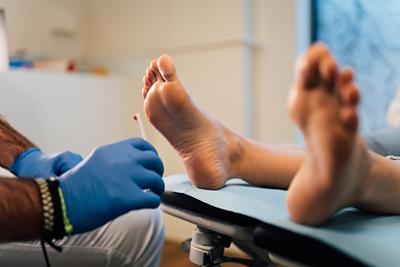
Diabetic Foot Care: Importance, Tips, and Warning Signs
posted: Apr. 07, 2024.

-
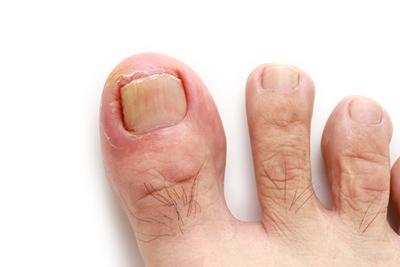
Symptoms of an Ingrown Toenail
posted: Apr. 01, 2024.
-
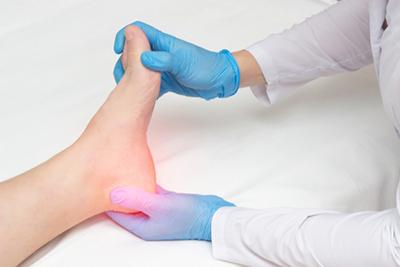
Treating Plantar Fasciitis
posted: Mar. 13, 2024.
-
Managing Your Heel Pain
posted: Mar. 01, 2024.
-
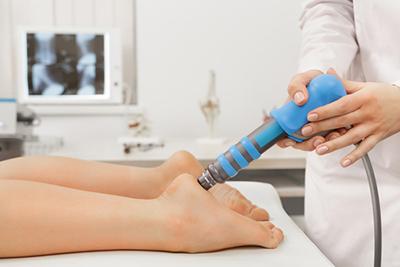
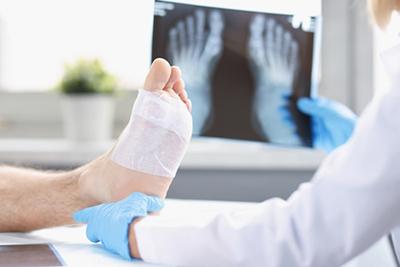
The Role of Podiatry in Managing Foot and Ankle Fractures
posted: Feb. 15, 2024.
-
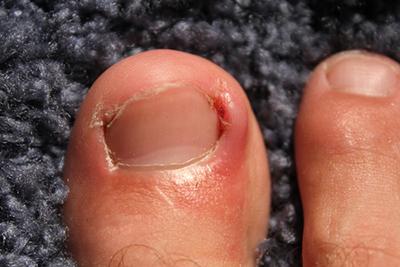
Ingrown Toenail Infections: Recognizing Signs and Seeking Prompt Treatment
posted: Feb. 12, 2024.
-
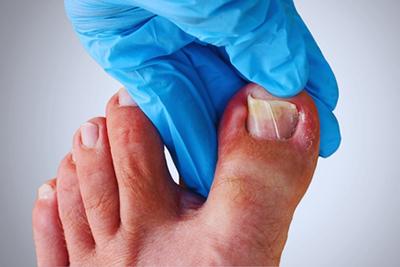
What You Need To Know About Ingrown Toenails
posted: Feb. 01, 2024.
-
Sports Podiatry: Addressing Foot and Ankle Injuries in Athletes
posted: Jan. 15, 2024.

-
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
posted: Jan. 01, 2024.

-
Non-Surgical Bunion Treatment Options: Orthotics, Splints, and More
posted: Dec. 22, 2023.

-
Diabetic Foot Care: Preventing Complications and Maintaining Foot Health
posted: Dec. 07, 2023.

-
Preventing Foot Injuries: Tips for Proper Foot Care and Injury Avoidance
posted: Dec. 01, 2023.

-
The Benefits of Seeing a Podiatrist
posted: Nov. 15, 2023.

-
The Benefits Of Orthotics
posted: Nov. 15, 2023.

-
When To See a Podiatrist
posted: Oct. 04, 2023.

-
The Importance of Diabetic Care
posted: Sep. 26, 2023.

Contact Us
Our Location
Find us on the map
Hours of Operation
Our Regular Schedule
Primary Location
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-5:00 pm
Wednesday:
8:00 am-5:00 pm
Thursday:
8:00 am-5:00 pm
Friday:
Closed
Saturday:
Closed
Sunday:
Closed